Do Stents Make You Feel Better?

The logic of stenting obstructed coronary arteries is simple.
The artery is blocked.
A stent unblocks the artery.
All is fixed.
If only it were that simple.
Stenting stable coronary artery disease has not been convincingly proven to reduce the risk of future heart attacks or death1.
However, the devil is in the detail when considering this question, and I have discussed it in more detail here.
What About Symptoms?
Whether stenting a narrowed coronary artery improves symptoms such as chest pain (angina) or shortness of breath is a very different question.
This is not about making you live longer; it is about making you feel better.
And again, the answer to this question looks pretty straightforward.
You have pain in your chest when you walk because of a narrowed coronary artery; you fix the artery with a stent, and voila, you feel better.
This was the prevailing opinion for many years, but two pivotal studies have added far more complexity to this question than we once thought.
Angina
The classic definition of angina involves the sensation of tightness in the centre of the chest that is brought on with exertion and is relieved with rest. There are many ways it can present but this is the most common.
The cause of angina usually involves inadequate blood flow reaching the heart muscle because of significant narrowing of the artery due to plaque buildup.

Stenting this segment of the vessel improves blood flow, so, therefore, it should reduce anginal symptoms.
But coronary stenting is not the only way to reduce symptoms of angina. Multiple medications have also been shown to improve symptoms.
ORBITA
The question then arises whether stenting or medications are equally effective at improving symptoms.
The ORBITA trial published in 2017 attempted to answer this question by taking people with significant narrowing of a coronary artery and then randomising them to either medications alone in addition to a sham procedure or medications plus stenting2.
Most importantly, patients were unaware if they had received a stent during their procedure.
The result of this trial sent shockwaves through the world of cardiology.
After six weeks, there was no difference in angina symptoms or exercise capacity between these two groups.
Had this elegant study put a nail in the coffin of coronary artery stenting?
Coronary stenting had now shown no major benefits in terms of reducing hard events like heart attacks and death, but its last stronghold was in symptom relief, and now this had failed.
Or had it?
ORBITA 2
One of the MANY criticisms of the original ORBITA trial was that the patients enrolled were very aggressively managed with multiple patient visits to get symptoms under control using multiple anti-anginal medications.
Many cardiologists felt this approach would not be feasible in the real world.
Others felt that the real question of whether the anti-anginal effect of stenting was a true placebo effect was not fully addressed, given that both groups were on maximal medical therapy.
So a follow-up trial called ORBITA 2 addressed this exact question and STOPPED the anti-anginal medications of patients with severe obstructive coronary disease and once again randomised patients to either a stent or a sham procedure where the patient was sedated and did not receive a stent3.
Both groups were unaware if they had received a stent or not.
The world of interventional cardiology collectively held its breath.
The result?
After 12 weeks, the coronary stenting group (PCI) had significantly fewer angina symptoms.
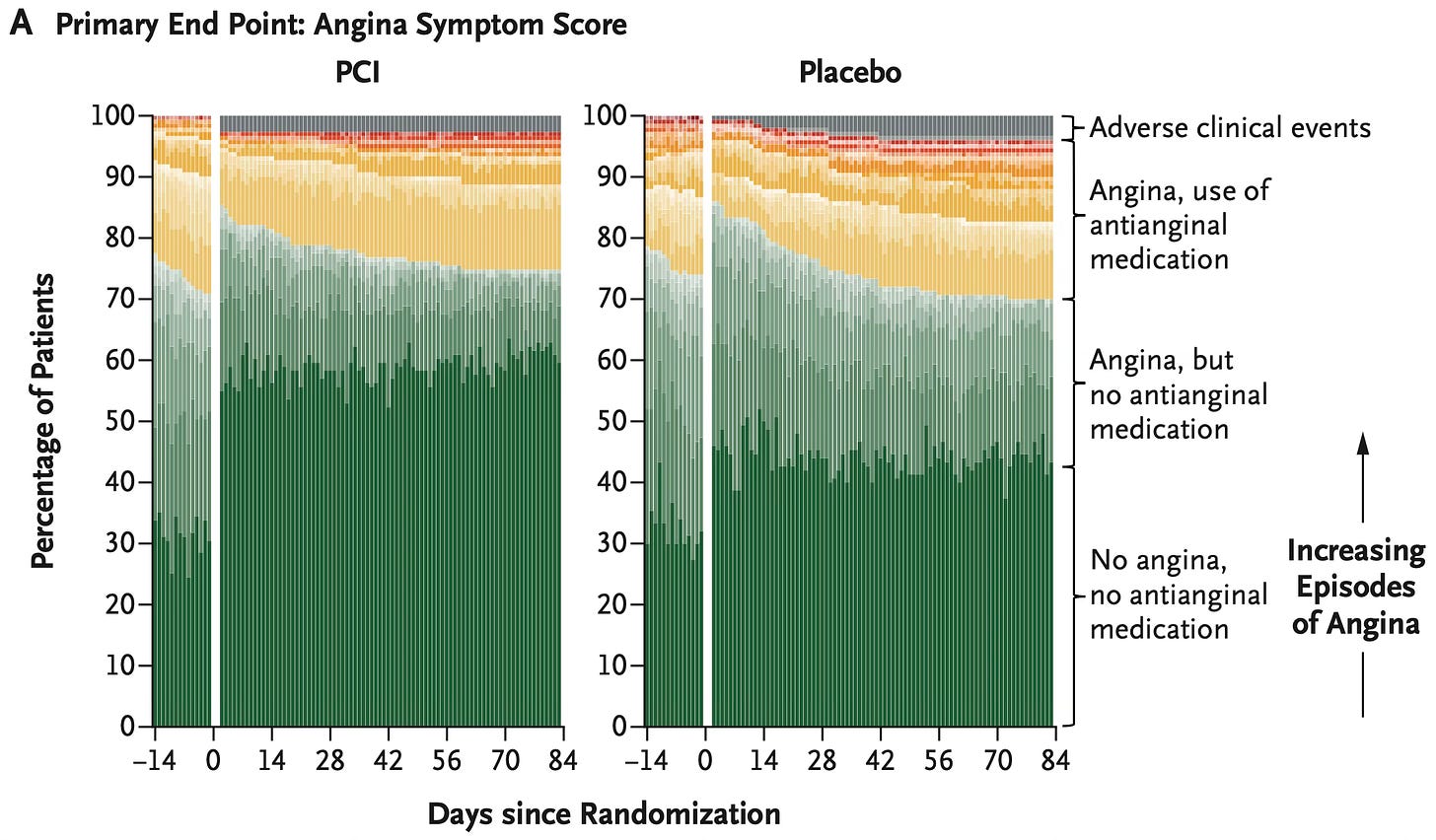

Finally, a win for coronary stenting.
But, as ever, the devil is in the details.
The above graphics clearly illustrate the differences in angina symptom scores and the number of anginal episodes, with significantly fewer occurring in the stenting (PCI) group.
However.
About 40% of the patients in the placebo group required no anti-anginal medications after having ALL of them stopped.
While fewer patients in the stenting arm had ongoing anginal episodes, many of them continued to have sometimes daily symptoms.
For sure, coronary stenting improves the symptoms of angina, but what is clear is that many patients continue to have symptoms despite coronary intervention.
This could mean these patients have very difficult-to-control symptoms, or symptoms that are not amenable to stenting (e.g. very small vessel disease), or symptoms that are not angina at all (We just happen to wrongly think it is)
What To Do?
There are some very important takeaways from these trials.
-
Anti-anginal medications are as good as coronary stenting in treating the symptoms of angina. The downside is you may need a lot of them, but the upside is that you are not exposed to the risk of an invasive procedure and the ongoing additional need for blood thinning medications.
-
Stenting is effective at reducing anginal symptoms, and the effect is not simply a placebo effect.
The bottom line is that there are advantages and disadvantages to either strategy.
Only you can decide with your cardiologist which is appropriate for you.
Even if you decide to go with a medications-only strategy, you can always revert to a stenting strategy if you are not making acceptable progress.
You cannot do it the other way around, though.
Both are equally effective and safe strategies for reducing the symptoms of angina.
However, neither has been shown to prevent heart attacks or make you live longer.
This is all a question of symptoms and quality of life.
But sometimes, that is a far more important issue.
ISCHEMIA Research Group. Initial Invasive or Conservative Strategy for Stable Coronary Disease. N Engl J Med. 2020 Apr 9;382(15):1395-1407.
ORBITA investigators. Percutaneous coronary intervention in stable angina (ORBITA): a double-blind, randomised controlled trial. Lancet. 2018 Jan 6;391(10115):31-40.
A Placebo-Controlled Trial of Percutaneous Coronary Intervention for Stable Angina. NEJM November 11, 2023




