Do You Need A Stent To Treat Your Heart Disease?

One of the most common questions I get is, “Do I need a stent to treat my heart disease?”
Typically, several of this person’s friends have had stents, so it seems natural to ask.
First, we must understand what a stent is and why it is used.
A stent is a metal scaffold deployed in a coronary artery that has reduced flow in that artery to restore flow.
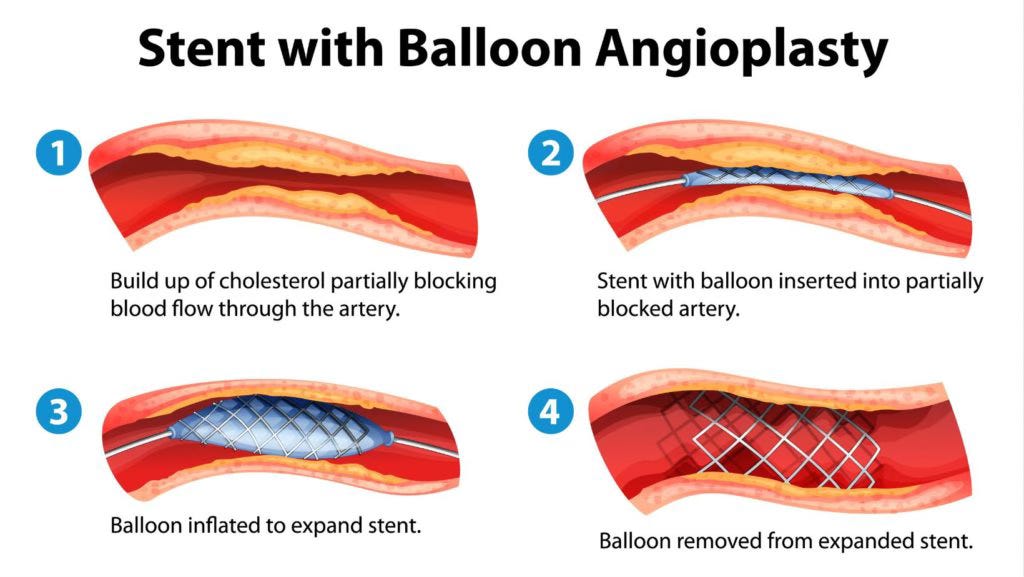
Seems pretty simple and makes total sense.
The artery is blocked.
The stent ‘unblocks’ it.
Flow is restored.
Of course, this all seems like a good idea.
But the devil is in the detail.
Why do arteries block?
Arteries generally narrow and occlude for one of two reasons:
-
The progressive accumulation of plaque.
-
A plaque ruptures, and a clot forms in the artery, thereby occluding it.
The second reason is commonly referred to as a ‘Heart Attack’ or acute coronary syndrome.
This is an emergency and is most often treated with a stent to restore blood flow in the artery.
The decision to use a stent here is usually clear and is associated with fewer deaths and heart attacks1.
In general, there is no debate here regarding the need for stenting a coronary artery.
Stenting In Stable Coronary Artery Disease
The real debate relates to the role of stenting in the setting of a severely narrow coronary artery outside the setting of a heart attack.
This is what is called stable obstructive coronary disease.
You have all heard the story.
“Johnny got checked or had some symptoms, and he needed a stent.”
The artery is blocked. The artery is now open.
Makes total sense.
But let’s take a closer look.
One of the first major studies to examine this question was the COURAGE trial, which took patients with significant coronary artery disease as evidenced by arteries that were at least 70% narrowed and tested whether medications or medications PLUSstenting would improve outcomes2.
The result?
After 4.6 years, there was no difference between these two groups in terms of death from any cause or heart attacks.
This was a major surprise.
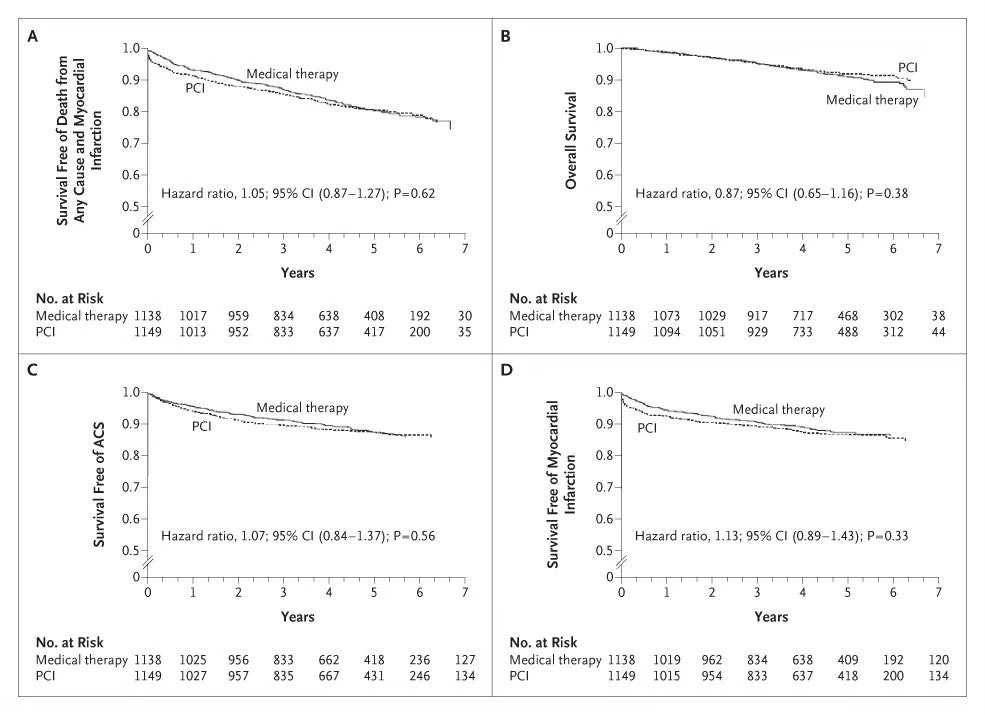
These patients had significantly narrowed arteries, and the use of a stent had no impact on what are referred to as hard outcomes: death, heart attack, etc.
There were, however, many criticisms of this trial, which we will not get into here, but broadly, this finding was not widely adopted into clinical practice for a variety of reasons.
Ischemia Trial
In an attempt to clarify this question, a similar trial was done called the Ischemia Trial, which had important differences to the Courage trial but again tried to answer a similar question3.
Does stenting severe stable obstructive coronary artery disease improve outcomes in terms of deaths or heart attacks?
The answer?
After three years, there was no difference in deaths or a combination of major heart events, including heart attacks.
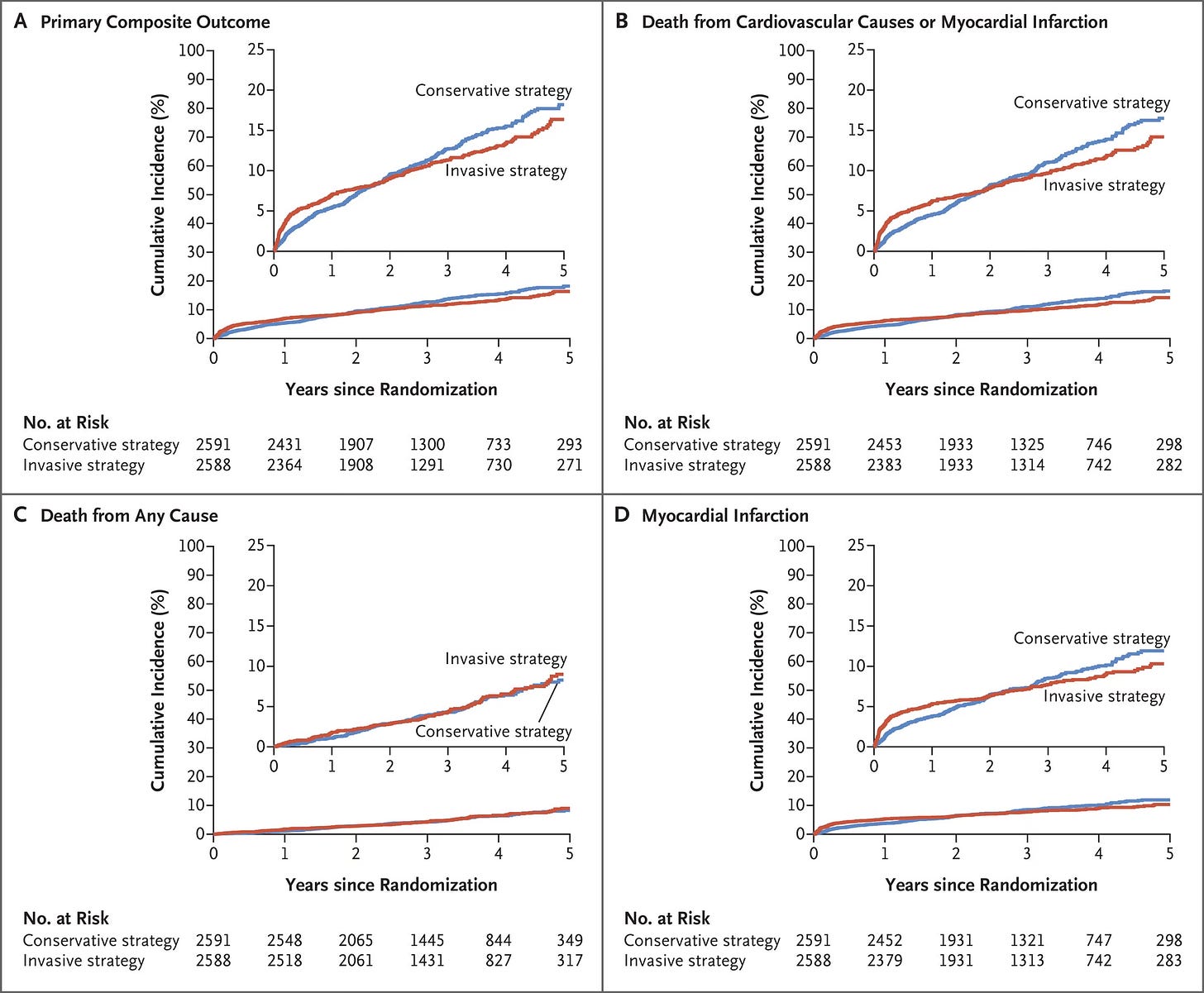
So it is now clear that outside of a heart attack, stenting obstructive coronary artery disease did not:
-
Make you live longer.
-
Prevent you from having a future heart attack.
This was another major finding in the world of cardiology.
However.
There has been significant debate about this trial that is too much to get into here, but to summarise one core issue that arose:
There are multiple types of heart attacks.
There are the ‘garden variety’ heart attacks whereby a plaque ruptures in the coronary artery, called a spontaneous heart attack. There are also heart attacks that can be caused by the stenting procedure itself, called periprocedural heart attacks.
In the group who were stented, there were MORE of the periprocedural heart attacks (as you would expect) but FEWER of the spontaneous heart attacks.
This finding, however, cannot be accepted at face value as this is not what the study was designed to look at, and therefore, the statistics used are not suitable.
Sorry. I know this is confusing. The joys of statistics.
But…
The bottom line is people did not live longer and did not have fewer heart attacks in total when stenting was used.
It is very easy to land on one side of this debate or the other and be rigid in your opinions.
It is easy to say stenting does not save lives or prevent heart attacks, and you would be right.
It is also easy to point out many elements of this trial that are worthy of discussion and potentially future studies that may change this finding.
What do I think?
When I have a patient with obstructive coronary artery disease, I ensure they:
-
Have all their risk factors addressed
-
Are on all the appropriate medications
I then go over this data and am very clear about the evidence.
For many, that is enough; we stick with medications, and I explain that if “Things change, we will change” and that choosing this option is not harmful.
Some patients really wish to have the narrowing addressed, and for those people, I highlight all the gaps in our knowledge, explain the risks, and proceed accordingly with stenting.
This works out well most of the time. But sometimes it doesn’t.
And the potential bad outcomes here include death.
At a minimum, it requires the implantation of a foreign metal object in your artery and also taking two potent blood thinners for at least six months.
I believe this situation requires careful conversation and an honest explanation of what the data says and where the gaps in our knowledge are.
For most, I encourage medical therapy alone.
But what about those with symptoms such as chest pain or shortness of breath as a result of their coronary artery disease?
This is a very different area than the hard outcomes of heart attacks, etc, but is about quality of life and symptom control.
That is what next week’s article dives into.
And you guessed it.
It’s not exactly straightforward.
And what we have learned recently has strongly informed my views on this topic, so stay tuned.
Arnold SV. Current Indications for Stenting: Symptoms or Survival CME. Methodist Debakey Cardiovasc J. 2018 Jan-Mar;14(1):7-13. doi: 10.14797/mdcj-14-1-7. PMID: 29623167; PMCID: PMC5880567.
COURAGE Trial Research Group. Optimal medical therapy with or without PCI for stable coronary disease. N Engl J Med. 2007 Apr 12;356(15):1503-16.
ISCHEMIA Research Group. Initial Invasive or Conservative Strategy for Stable Coronary Disease. N Engl J Med. 2020 Apr 9;382(15):1395-1407.




