The Value Of Lifestyle In Those With An Elevated Lp(a)

An elevated Lp(a) is a common genetic factor that is independently and causally related to premature coronary artery disease.
But we must always remember that most genetic risk factors are probabilistic rather than deterministic in terms of risk.
The distinction here is crucial, as most of the early work on genetics and risk has led us astray.
Here’s why.
Gregor Mendel was a German Augustinian Friar who laid the basis of our understanding of genetics with his work on pea plants.
His work provided us with the concepts of the inheritance pattern of genetic factors.

For example, an autosomal dominant trait meant that if a parent had this genetic trait, there was a fifty-fifty chance a child would inherit it and that child would have the disease associated with it.
Think Huntington’s Disease or Marfan’s Syndrome.
If the condition were autosomal recessive, you would have to inherit a copy of the gene from both parents to end up with the condition. In this instance, if both parents had a copy of the disease gene, there would be a one in four chance that the child would have the disease.
The probabilities were quite clear.
But that is not how genetic determinants of risk usually work.
While the gene variants that cause an elevated Lp(a) are indeed inherited in an autosomal dominant fashion, whether or not someone develops the condition associated with it, i.e. early heart disease, is not so clear cut.
The occurrence of disease in this instance is probabilistic, not deterministic.
i.e. you can increase and decrease the odds of it being an issue for you.
This is the case with an elevated Lp(a).
In my experience, some patients present later in life with a significantly elevated Lp(a) but have no evidence of coronary artery disease.
They have the biomarker of risk but no evidence of the disease, even later in life when you would expect them to have it.
Why?
Firstly, there is definitely something about the family history that matters.
When there is a history of early events, then the likelihood of a member of that family with an elevated Lp(a) having premature coronary atherosclerosis is high.
Conversely, even when levels of Lp(a) are high, when the family history is not suggestive of early heart disease, then the likelihood of that person having early heart disease seems to be low.
This is, of course, anecdotal evidence, but it does seem that other factors are at play.
Is lifestyle one of those factors?
The answer, it seems, is yes.
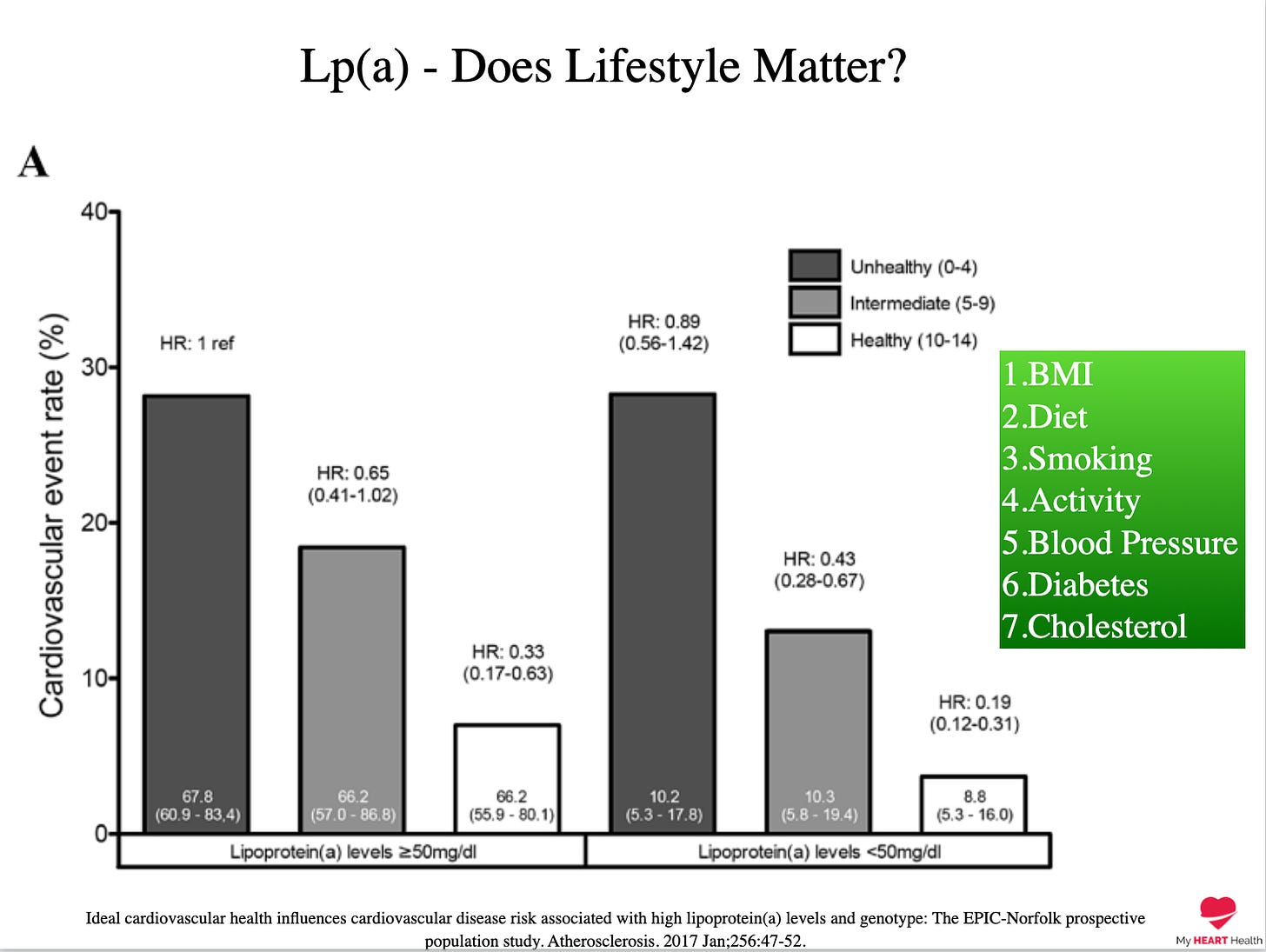
If you separate those with a significantly elevated Lp(a) (>50mg/dl) and a normal Lp(a) by levels of healthy lifestyle, you see major differences in outcomes.
A healthy lifestyle, in this instance, is defined by a combination of:
-
BMI
-
Nutrition
-
Smoking Status
-
Activity Levels
-
Blood Pressure
-
Diabetes Status
-
Cholesterol Levels
All of which are highly modifiable.
Compared to those with an elevated Lp(a) who scored low on the lifestyle scale, those with an elevated Lp(a) who scored high on the lifestyle scale had 63% less likelihood of a cardiovascular event1.
For those without an elevated Lp(a) and a high score on the lifestyle scale, the reduction in risk was 81%.
Which means two things:
-
A healthy lifestyle, even in the presence of an elevated Lp(a), can significantly reduce cardiovascular risk.
-
Even with a healthy lifestyle, there is still incremental risk associated with an elevated Lp(a), but it is relatively modest in comparison.
The key takeaway here is that the risk is probabilistically adjusted based on lifestyle factors.
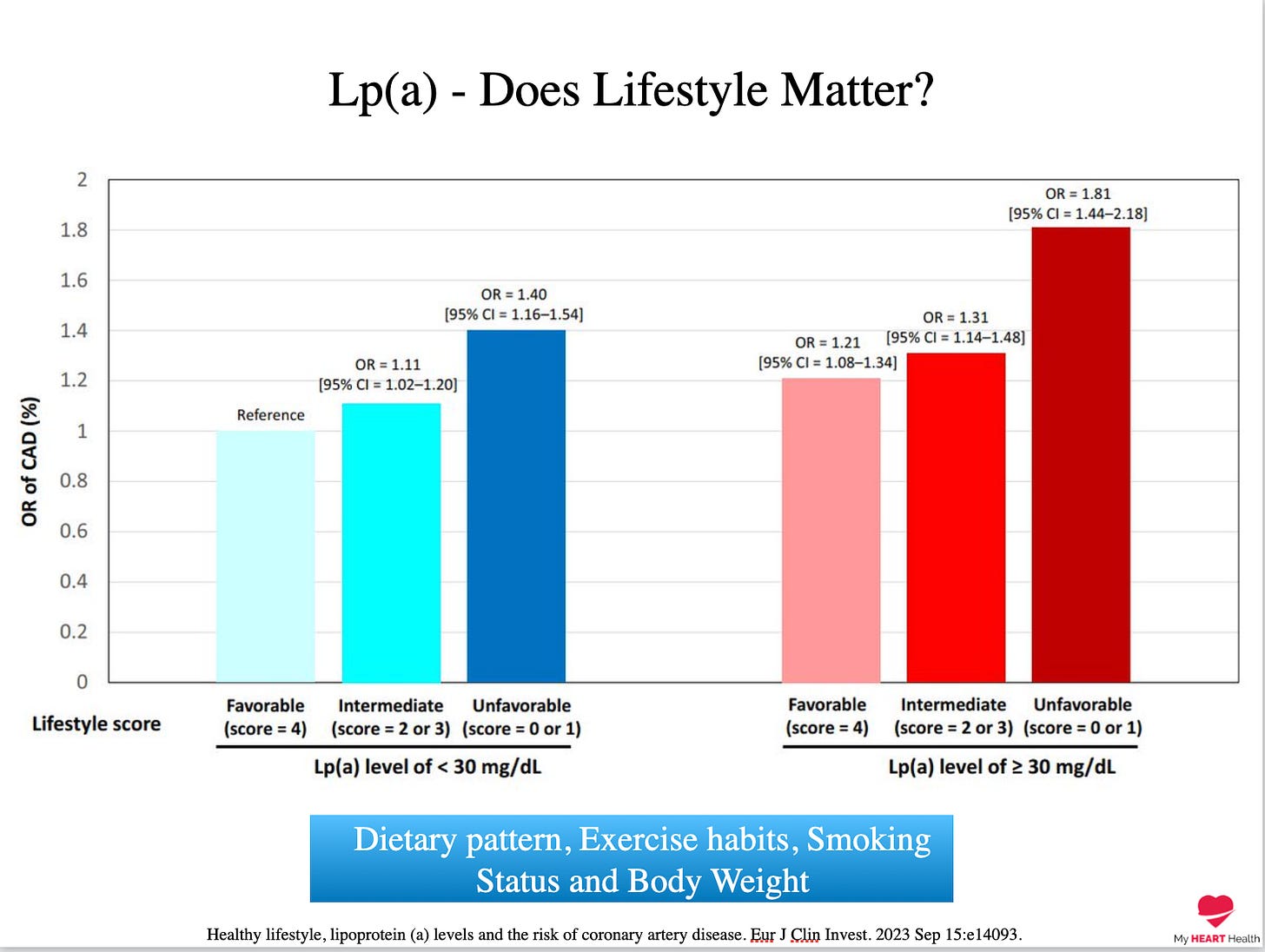
But what about Lp(a) levels greater than 30mg/dl?
Some labs report incremental risk only with levels above 50mg/dl, but it is becoming increasingly clear that even levels above 30 mg/dl can confer incremental risk.
A different study looked at this very question, and again, the trend is the same.
Better lifestyle factors significantly reduced the risk of coronary artery disease, but even with an optimal lifestyle pattern, there was a small increase in risk2.
An elevated Lp(a) does increase the risk of early cardiovascular disease, but that risk is not set in stone.
It is probabilistically adjusted based on the lifestyle factors of the individual.
There is currently no approved therapy to selectively lower Lp(a) levels, but it is essential to understand that just because we cannot lower Lp(a) levels does not mean we cannot lower risk.
The latter is arguably far more important.
Because there is no approved therapy to lower Lp(a), many clinicians feel that measuring Lp(a) levels is of no value.
I could not disagree more.
Sometimes, we need to see that we are at higher risk to motivate us to make the changes necessary to reduce our risk via lifestyle measures.
These studies highlight the fact that with optimal lifestyle factors, the risk of early heart disease can be mitigated.
Genetics matter, but their impact on risk can be modified.
Most of the chronic medical conditions we deal with today do not follow the Mendelian patterns of inheritance and disease. However, we still tend to think of most genetic issues as acting this way, which is incorrect.
As the line goes:
“Genes load the gun, and lifestyle pulls the trigger.” - Caldwell Esselstyn
With an elevated Lp(a), you may have a loaded gun, but only you can decide whether or not to pull the trigger.
Ideal cardiovascular health influences cardiovascular disease risk associated with high lipoprotein(a) levels and genotype: The EPIC-Norfolk prospective population study. Atherosclerosis. 2017 Jan;256:47-52.
Healthy lifestyle, lipoprotein (a) levels and the risk of coronary artery disease. Eur J Clin Invest. 2023 Sep 15:e14093.




